Understanding Venous Insufficiency
What Is Venous Insufficiency?
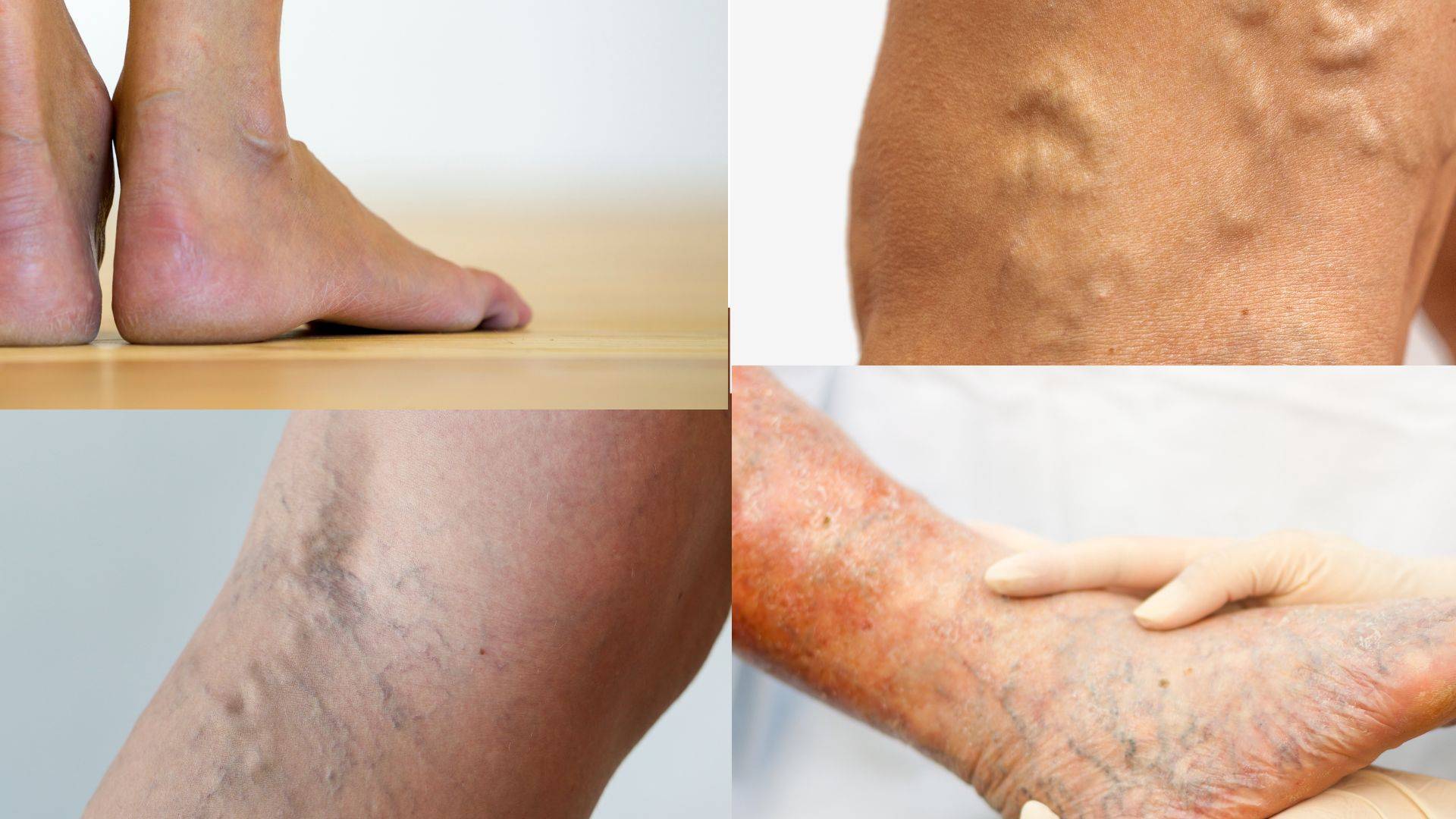
Venous insufficiency is a chronic condition where the veins in your legs can’t efficiently return blood to your heart. This leads to blood pooling, causing swelling, discomfort, and visible varicose veins. It’s more common than many think and affects millions worldwide, particularly as they age.
How Veins Normally Work
Your veins rely on one-way valves and muscle contractions to push blood upward against gravity. In venous insufficiency, these valves become weak or damaged, allowing blood to flow backward and pool in the lower legs.
Causes of Venous Insufficiency
- Valve Damage: Often due to age or previous blood clots.
- Prolonged Standing or Sitting: Common in jobs like teaching, nursing, and office work.
- Pregnancy: Increased blood volume and hormonal changes put pressure on leg veins.
- Obesity: Excess weight puts added strain on veins.
Symptoms to Watch Out For
Early Warning Signs
- Heavy, aching legs
- Visible varicose veins
- Leg cramps, especially at night
Chronic Symptoms
- Swelling in ankles and calves
- Itchy, flaky skin near affected veins
- Discoloration or darkening of the skin
When to Seek Medical Attention
If symptoms persist for more than a few weeks or worsen with time, consult a vascular specialist. Untreated venous insufficiency can lead to serious complications like leg ulcers or deep vein thrombosis (DVT).
Risk Factors and Who’s Most Affected
Age and Gender Differences
Women over 50 are at higher risk due to hormonal shifts and pregnancy history. However, men are increasingly diagnosed due to lifestyle changes.
Lifestyle and Occupation
Jobs that require prolonged standing or sitting increase risk. Airline crew, surgeons, and retail workers often face challenges.
Genetic and Medical Conditions
A family history of vein problems or clotting disorders can raise your risk. Other health issues like hypertension or diabetes also contribute.
Diagnosis and Evaluation
Medical History Review
Your doctor will ask about symptoms, family history, pregnancies, and lifestyle habits to identify contributing factors.
Physical Examination
Swelling, skin changes, and visible varicose veins are usually noticeable during a clinical exam.
Diagnostic Imaging Tests
- Duplex Ultrasound: The gold standard for diagnosis
- Venogram: Used in complex cases
- Photoplethysmography: Measures blood flow and pressure in the legs
Lifestyle Changes to Improve Symptoms
Daily Habits to Help Circulation
- Elevate your legs several times daily
- Avoid standing or sitting for long periods
- Shift positions often
Foods That Support Vein Health
- High-fiber foods to reduce pressure
- Flavonoid-rich fruits like berries
- Leafy greens and hydration to prevent swelling
Exercise Tips for Better Blood Flow
- Walking: 30 minutes a day improves calf muscle pump
- Leg lifts and ankle rolls: Easy home exercises
- Swimming: Low-impact, circulation-boosting option
Compression Therapy
How Compression Stockings Work
These snug-fitting garments apply pressure to your legs, helping veins move blood more efficiently toward the heart.
Types of Compression Garments
| Type | Use Case |
|---|---|
| Mild (8-15 mmHg) | Mild swelling or pregnancy |
| Moderate (15-20 mmHg) | Daily use or travel |
| Strong (20-30+ mmHg) | Chronic venous disease, post-surgery |
When and How to Use Them
Wear them during the day, especially when active or sitting for long periods. Always consult a physician for the correct fit and grade.
Medications for Venous Insufficiency
Topical and Oral Medications
- Topical creams for itching and inflammation
- Diosmin-based supplements improve vein tone
Anti-inflammatory and Anticoagulant Use
- NSAIDs reduce pain and inflammation
- Blood thinners prevent clot formation
Benefits and Side Effects
While medications can relieve symptoms, they often work best when combined with other therapies like compression and exercise. While these help symptoms control of root causes for lasting treatment requires procedural intervention.
Minimally Invasive Procedures
Endovenous Laser Ablation (EVLA)
A laser is inserted into the vein, sealing it from within. It’s highly effective with minimal downtime.
Radiofrequency Ablation (RFA)
Similar to EVLA, but uses radio waves instead of laser heat. Effective in sealing large varicose veins.
Adhesive Injections
Similar to RFA but utilizing adhesive to close veins. Advantages with treatment allows for inclusions of diseased vein segments that cannot be safely treated by heat.
Surgical Treatments
Vein Stripping and Ligation
Outdated but still used in severe cases. The vein is tied off and removed through small incisions.
Ambulatory Phlebectomy
Small surface veins are removed via micro-incisions—no stitches needed, and minimal scarring.
When Is Surgery Necessary?
Surgery is recommended if less invasive methods fail, or if complications like ulcers and clots arise.
Natural Remedies and Holistic Approaches
Herbal Treatments and Supplements
- Horse chestnut extract reduces inflammation
- Butcher’s broom supports vein tone
Massage and Elevation Techniques
Manual lymphatic drainage and elevating legs can relieve swelling and fatigue.
Acupuncture and Alternative Therapies
Some patients report improvement with acupuncture, reflexology, and ayurvedic herbs—though more research is needed.
Managing Pain and Swelling
Cold vs. Heat Therapy
Cold compresses reduce swelling. Warm baths help relax vein walls and reduce cramping.
Pain-Relief Techniques at Home
- Elevation
- Compression
- Massage with essential oils (lavender, peppermint)
When to Use OTC Medication
Use ibuprofen or acetaminophen sparingly for relief, always checking with your doctor first.
Preventing Future Complications
Long-Term Care Plans
- Regular follow-ups with your vein specialist
- Daily use of compression garments
- Continued exercise and weight management
Preventive Screenings
Annual vascular exams for high-risk individuals can detect early changes.
Managing Coexisting Conditions
Control diabetes, blood pressure, and cholesterol to reduce vascular strain.
Living Well with Venous Insufficiency
Emotional and Mental Health Impact
Chronic pain and visible veins can affect self-esteem and mood. Seeking support is key.
Support Groups and Counseling
Online and in-person groups offer shared experiences and coping strategies.
Building a Sustainable Routine
Create a daily schedule that includes:
- Morning walks
- Compression wear
- Leg elevation breaks
Success Stories and Real Patient Experiences
Inspiring Recoveries
Many patients report walking pain-free within weeks after Treatment or instituting conservative measures.
Challenges and Breakthroughs
From struggling with long flights to climbing mountains post-recovery, real-life triumphs inspire others.
Lessons Learned from Others
Stay consistent with treatment. Avoid quick fixes. Trust medical advice, and stay informed.
Frequently Asked Questions (FAQs)
1. Can venous insufficiency go away on its own?
No. It typically worsens over time without treatment. Lifestyle changes and therapies help manage it.
2. Is walking good for venous insufficiency?
Yes. Walking activates calf muscles, promoting blood flow upward and relieving symptoms.
3. What are the best compression socks for venous insufficiency?
Medical-grade (20-30 mmHg) knee-high socks are most effective. Always consult a doctor for sizing. As the disease worsens know that the venous pressure can and usually goes up. When it exceeds 30 mmHg you have to wear tighter stockings or have a procedure or the disease will worsen.
4. What happens if I leave venous insufficiency untreated?
You risk developing skin ulcers, deep vein clots, and permanent leg discoloration. Additionally you may inhibit natural perfusion thereby inhibiting optimal muscle function… you feel tired.
5. Are natural treatments as effective as medical ones?
They can support medical care but are rarely effective on their own in moderate to severe cases.
6. Can I fly with venous insufficiency?
Yes, with precautions: wear compression socks, walk while on the flight, and stay hydrated. Consider a baby aspirin or Omega-3 fish oil.
Conclusion: Your Path Forward in Treating Venous Insufficiency
Dealing with venous insufficiency and treatment options doesn’t have to be overwhelming. With early diagnosis, proper care, and a mix of medical and lifestyle strategies, you can reclaim comfort and confidence in your legs. Don’t wait—talk to a vein specialist today and take your first step toward healthier circulation.